If you've had your Lp(a) measured, you've already taken a step that most Canadians haven't. A clinical framework published this month in the Canadian Journal of Cardiology highlights the importance of knowing your Lp(a) and provides guidance about what to do with the result.
What is Lp(a)?
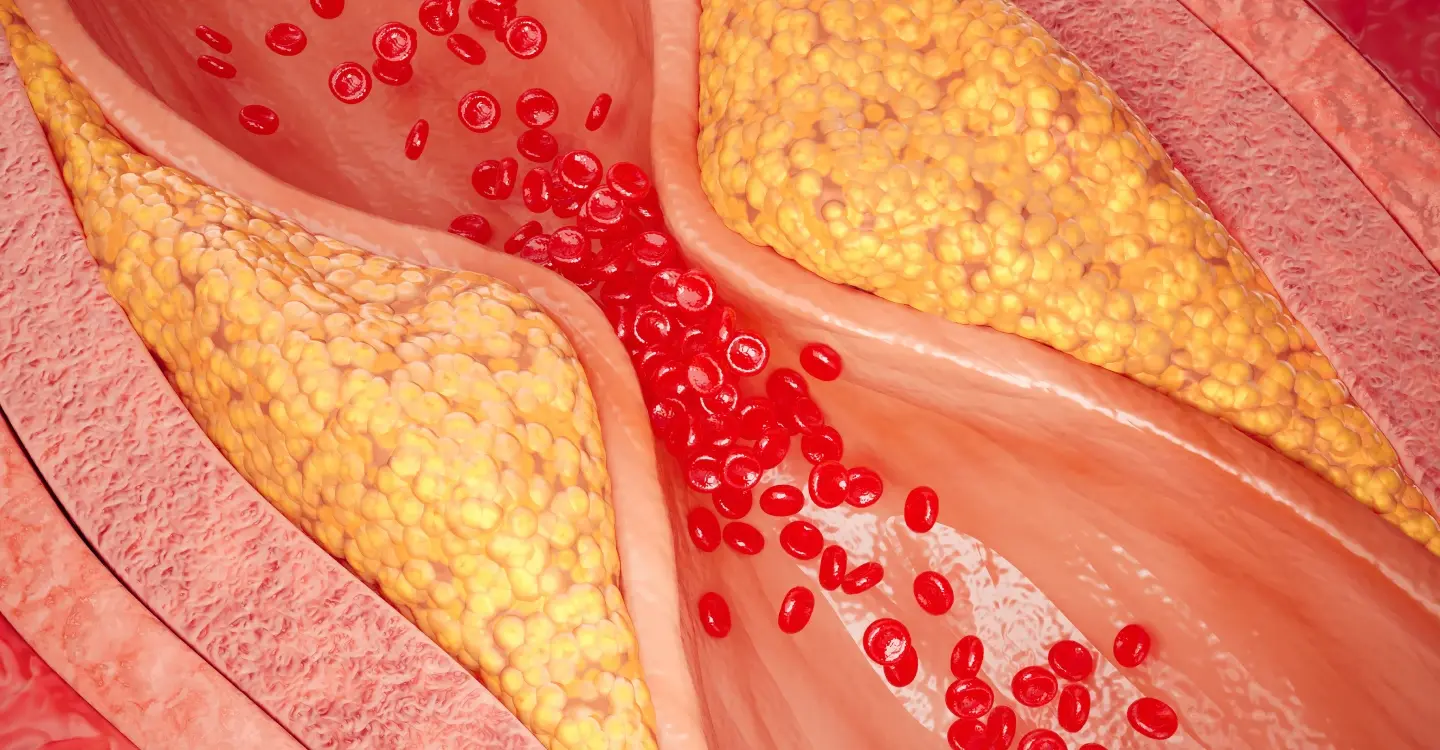
Lipoprotein(a) — written as Lp(a) and pronounced "L-P-little-a" — is a cholesterol-carrying particle in your blood. Structurally similar to LDL ("bad cholesterol"), it carries an additional protein called apolipoprotein(a), which makes it particularly dangerous. Lp(a) promotes atherosclerosis (plaque buildup in arteries), increases the tendency of blood to clot, and drives inflammation in blood vessels.
What makes Lp(a) unusual among cardiovascular risk factors is that it is almost entirely determined by your genes — more than 90% of the variation in Lp(a) levels between people is genetic. That means diet, exercise, and most standard cholesterol medications have very little effect on it. Your Lp(a) level is largely set at birth, and it stays relatively stable across your adult life.
Despite this, Lp(a) isn't a sentence. It's information — and the right information allows for smarter, more targeted prevention.
Why does Lp(a) matter?
Elevated Lp(a) increases the risk of several serious conditions, including heart attack, stroke, peripheral artery disease, and calcific aortic valve stenosis (a narrowing of the heart's main outflow valve). The relationship between Lp(a) and cardiovascular risk is continuous and dose-dependent — the higher the level, the higher the risk.
On a per-particle basis, Lp(a) appears to be approximately six times more atherogenic than LDL. That's a striking figure, and it helps explain why people can have "normal" LDL cholesterol and still develop early or severe cardiovascular disease.
Lp(a) is elevated in roughly 1 in 5 Canadians — an estimated 8 million people. Yet fewer than 1 in 10 high-risk individuals have ever been tested for it.
What the new guidance says
A multidisciplinary working group of leading Canadian cardiologists, endocrinologists, family physicians, pharmacists, and basic scientists published a comprehensive clinical framework for managing Lp(a) in Canada. The paper, led by Dr. George Thanassoulis of McGill University and colleagues at institutions across the country, provides guidance on who should be tested, how results should be interpreted, and what should be done when Lp(a) is elevated.
Here are the most important takeaways.
1. Universal, one-time testing is recommended for all adults
The working group formally endorses universal Lp(a) measurement — once in adulthood, ideally at the time of a first lipid panel, around age 40. Those with a family history of premature heart disease or other risk factors should be tested earlier.
This recommendation is already made by the Canadian Cardiovascular Society (CCS) and major international cardiovascular bodies. Yet the new framework acknowledges frankly that universal screening remains "aspirational" in Canada — with only around 10% of high-risk individuals currently receiving the test.
This is a significant gap. Lp(a) is one of the few cardiovascular risk factors that is both common and substantially underdiagnosed, despite being measurable with a single, inexpensive blood test.
NiaHealth has included Lp(a) as a standard component of our assessment panel from day one, across every panel of tests from Lite to ultra, precisely because we believe everyone deserves this information.
2. The at-risk threshold is ≥100 nmol/L
Lp(a) levels at or above 100 nmol/L (approximately 50 mg/dL) are considered elevated. Levels above 190 nmol/L are considered markedly elevated, and levels at or above 400 nmol/L confer a lifetime cardiovascular risk equivalent to that of familial hypercholesterolemia (a well-recognized genetic cholesterol disorder).
NiaHealth uses the same ≥100 nmol/L cutoff for our "at-risk" classification; flagging suboptimal levels at ≥75 nmol/L.
3. Women approaching menopause may need a repeat measurement
This is a nuanced but clinically important point. Lp(a) levels can increase by 20–30% during and after the menopausal transition. This means a result measured in premenopause may underestimate a woman's postmenopausal Lp(a) level.
If your Lp(a) is measured before menopause and is close to the 100nmol/L threshold, it is worth repeating the test in the postmenopausal period.
4. High Lp(a) is a family matter
Lp(a) levels are highly heritable. If one person in a family has elevated Lp(a), there is roughly a 1 in 2 chance that a first-degree relative (parent, sibling, or child) does too — and about a 1 in 3 chance for second-degree relatives (grandparents, aunts, uncles, cousins). Systematic testing of close biological relatives of anyone found to have elevated Lp(a) is recommended.
This is both a health imperative and an opportunity. Identifying elevated Lp(a) in a family member who doesn't yet know about it is one of the highest-yield things that can come from an individual's result.
5. Imaging may help clarify risk in select individuals
For those with markedly or extremely elevated Lp(a), certain imaging investigations can help quantify actual cardiovascular risk and inform management decisions:
Coronary artery calcium (CAC) scoring or coronary CT angiography (CCTA) can assess whether calcified or non-calcified plaque is already present in the coronary arteries. Importantly, the working group notes that a CAC score of zero does not fully rule out risk in the context of high Lp(a), because Lp(a) is more likely to produce non-calcified (vulnerable) plaque. CCTA may be more informative than CAC alone for younger individuals or those with very high Lp(a) as it can identify both calcified and non-calcified plaque build up.
Abdominal ultrasound is suggested for individuals over 60 with elevated Lp(a) to screen for abdominal aortic aneurysm — particularly in men and those who have ever smoked.
Echocardiogram is recommended for anyone with a systolic heart murmur, to detect aortic valve disease, which Lp(a) is known to drive through calcium deposition on the valve.
6. Management today focuses on overall cardiovascular risk reduction
No approved, targeted Lp(a)-lowering therapy exists (yet–see below). But the finding of elevated Lp(a) is far from a dead end. It is a signal to act decisively on every modifiable cardiovascular risk factor in your profile.
The areas to focus on are:
- A healthy diet high in complex carbohydrates, fibre, fish, and vegetables, 150 minutes of moderate physical activity per week, avoidance of tobacco, optimal sleep (7–9 hours), healthy weight, and strict control of blood pressure, blood sugar, and lipid levels
- Consider and optimize lipid-lowering medications — statins remain the first line treatment, but because treatment targets are lower in people with elevated Lp(a), additional medications (ezetimibe or a PCSK9 inhibitor) may be required
- Aggressive blood pressure control, targeting systolic blood pressure below 120 mmHg where tolerated
- For persons living with diabetes, prioritizing medications with established cardiovascular benefit
- An individualized discussion with your health care provider about low-dose aspirin, weighing cardiovascular benefit against bleeding risk
7. Lp(a)-specific therapies are coming
Several drugs in late-stage clinical trials including antisense oligonucleotides (Pelacarsen) and small interfering RNAs (Olpasiran, Lepodisiran, Zerlasiran) can reduce Lp(a) levels by 80–94%. The first cardiovascular outcomes trial results are expected this year and 2027.
If these trials are positive, they could transform the management of elevated Lp(a) in the same way statins transformed the management of elevated LDL. NiaHealth will continue to keep our members informed as these developments unfold.
What you should do now
If you've had your Lp(a) measured through NiaHealth: Log in to review your result and its interpretation in your dashboard. Share the result with your primary care provider at your next visit — many family MDs and NPs are still unfamiliar with Lp(a), and bringing in your result with the relevant reference range (e.g. ≥100 nmol/L = elevated) is a straightforward way to start the conversation.
If your Lp(a) is elevated:
- Talk to your family. Family screening is recommended.
- Work with your healthcare team or NiaHealth team to optimize every other modifiable risk factor.
- Ask whether your current lipid-lowering therapy is appropriately intensive given your Lp(a).
- If you are a woman past menopause repeat your test.
If you haven't yet completed your NiaHealth assessment: Now is a good time. Lp(a) is measured as part of every standard panel.
The bottom line
Lp(a) is one of the most common genetic risk factors for cardiovascular disease in Canada. The new guidance from Canadian cardiovascular experts is clear: every adult should be tested at least once, results should be used to guide risk stratification and prevention, and family members of affected individuals should be screened.
NiaHealth was built on the premise that everyone deserves access to this kind of proactive, evidence-based insight. This paper affirms that premise — and reinforces why knowing your Lp(a) is one of the most important things you can do for your long-term heart health.
Our editorial standards & process
At NiaHealth, our mission is to make proactive health possible for all Canadians—by combining science with humanity. We believe that rigorous, evidence-informed health information should never feel out of reach. Every word we publish is intentional. We choose language that empowers rather than overwhelms, clarifies rather than complicates, and respects the lived experiences behind every health question. Learn more here.